Prioritizing AI in the Digital Mailroom: Where Health Plans Should Start
By Vidhya Bhat, Chief Product Officer, Digital Transformation
For most health plans, the conversation about AI has already moved past why. Leaders understand the promise: faster processing, lower costs, better compliance. What’s more difficult—and far more operationally important—is deciding where to apply artificial intelligence first.
Within modern multi-modal intake workflows, the digital mailroom functions as the front door to the payer’s information ecosystem—and is often the most logical starting point for AI. It’s document-heavy, operationally complex, and full of manual work that feels ripe for automation. Yet it’s also where many AI initiatives stall. Not because the technology fails, but because everything is treated as equally urgent.
In reality, not every document type belongs at the front of the automation line. Prioritization is what separates early wins from long pilots that never quite deliver. Based on real-world health plan experience, here’s a practical way to think about where in the digital mailroom AI pays off first—and how to build momentum without overreaching.
Why “Automate Everything” Rarely Works
Health plans receive an enormous range of inbound documents—claims, appeals, provider letters, medical records, enrollment forms, returned mail—arriving through paper, fax, email, portals, and clearinghouses. Only a small fraction of that volume is clean, structured, and predictable.
When AI is applied too broadly, too fast, accuracy suffers on documents that aren’t ready for automation. Compliance risk increases when time-sensitive items aren’t identified early. And ROI becomes difficult to prove when effort outweighs operational impact.
The most successful teams take a narrower approach. They focus on the first mile of intake—classification, extraction, and routing steps that determine how quickly and accurately work moves downstream. In practice, this transforms the digital mailroom into a centralized intake engine that standardizes how information enters the organization.
Where AI Should Start in the Digital Mailroom
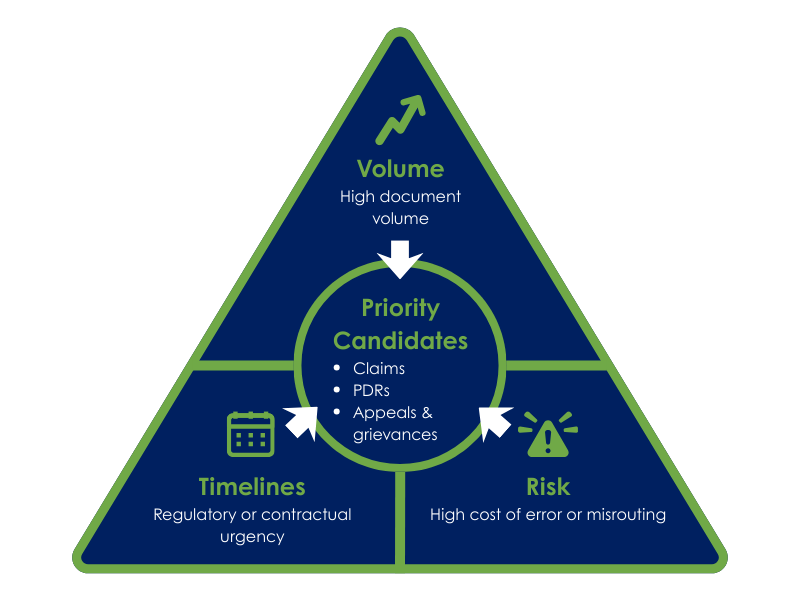
Prioritize document types where volume, timelines, and risk intersect.
Start Where Time, Volume, and Risk Intersect
Across health plans, certain document categories consistently rise to the top when leaders evaluate impact versus effort. These documents tend to share three traits: meaningful volume, regulatory or contractual timelines, and high cost when mistakes occur.
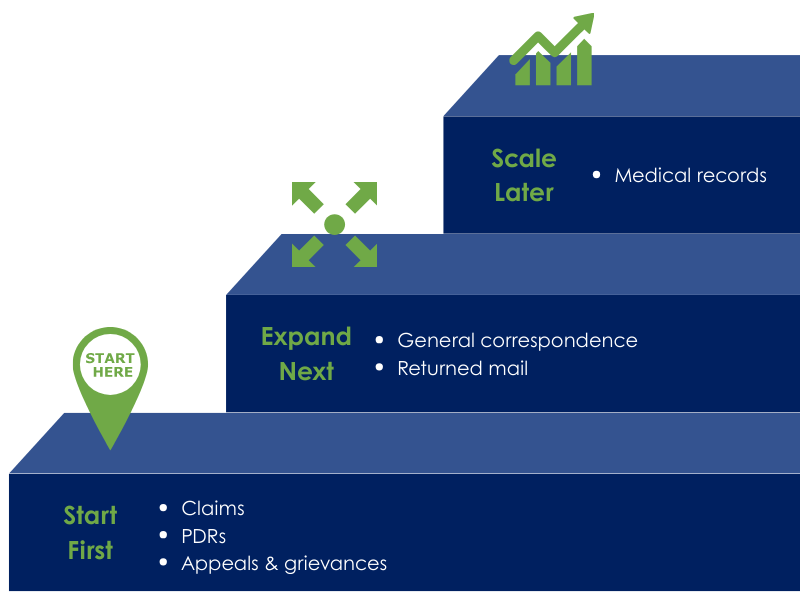
Claims are the most obvious starting point, given longstanding regulatory timelines and adjudication requirements. While they represent a minority of total inbound documents, HCFA and UB forms, for instance, carry outsized operational importance. They are highly standardized and familiar to the industry, which makes them ideal candidates for AI-driven classification and optical character recognition (OCR). When handled well, AI reduces downstream rework, improves adjudication timelines, and lowers the overall cost of quality.
Provider Dispute Resolution documents often follow. PDRs are time-sensitive and frequently misrouted, buried within general correspondence streams. AI’s ability to recognize patterns and intent—even when documents are inconsistently labeled—makes it especially effective at surfacing these items and routing them on time.
Appeals and grievances add another layer of urgency. These documents are less structured than claims, but they carry some of the highest regulatory exposure in health plan operations, particularly for Medicare Advantage and managed Medicare plans. Here, AI is less about full automation and more about risk control.
Where AI Begins to Unlock Scale
Once high-risk, time-sensitive documents are under control, AI-driven classification can start delivering value at scale through general correspondence—reducing manual sorting and stabilizing downstream workflows. This category often represents the largest share of inbound volume.
Documents arrive in the wrong mailboxes, through unexpected channels, and with little consistency in format or labeling. Traditional rules-based logic often struggles here, especially as document formats and language vary widely. AI, by contrast, excels at classification problems where context matters more than rigid templates. By identifying document intent—such as enrollment, eligibility, billing, or provider inquiry—AI reduces manual sorting and accelerates routing across the organization.
Returned mail also can offer some of the clearest early wins. Identifying returned correspondence and extracting address-related signals is a relatively straightforward application of AI, yet it delivers outsized impact. Improving address accuracy supports compliance, reduces downstream rework, and helps ensure critical member communications reach their destination.
Medical records typically come later in the scaling journey.
A Practical Path to AI Adoption in the Digital Mailroom
They are complex and resource-intensive, which makes them a poor starting point for most AI initiatives. But once capabilities such as classification and OCR are mature, AI can improve how records are indexed, retrieved, and reviewed—reducing friction for utilization management, audits, and provider follow-ups.
Designing Human Oversight Without Slowing Everything Down
A common misconception is that AI success depends on removing humans from the process.
However, most effective digital mailrooms use AI to focus human effort where judgment matters most. Reviewers concentrate on exceptions and high-risk categories instead of validating every document. Quality assurance becomes targeted rather than universal.
Progress Comes From Prioritization
AI in the digital mailroom isn’t about automating everything at once. It’s about stabilizing the front end of operations—reducing risk, cost, and delay where intake quality determines everything that follows.
Health plans that prioritize thoughtfully—starting with the right document types and expanding deliberately—tend to move faster, stay compliant, and realize value sooner.
Ready to See Where Intelligent Intake Fits into Your AI Roadmap?
Watch our on-demand webinar, Intelligent Intake for Digital Mailrooms, to learn how health plans apply AI to classification and extraction to drive early automation wins and scale operational efficiency.